
Is it possible to perform coronary bypass surgery without cutting the sternum? How long does it really take to recover? How will your health change after surgery? How long do they live after coronary bypass surgery?..
Cardiac surgeon Oleg Kozlov, head of the cardiac surgery department of the RCMC, answered readers' questions.
1. «My doctor said I need heart bypass surgery. I'm scared. Is there no way around this operation?»
— Coronary artery bypass grafting is performed for ischemic heart disease, which occurs when atherosclerotic plaques form in the heart arteries, either narrowing or blocking the vessel lumens from the inside.
Consequently, the heart and cardiac muscle receive less blood than needed, especially during physical and emotional stress.
When the heart requires oxygen and nutrients, blood cannot deliver them adequately through these narrowed vessel lumens.
In such cases, surgical treatment is necessary, either through stenting or coronary artery bypass grafting.
- During stenting, a spring-like device (stent) is inserted into the vessel lumen to expand it from the inside.
- In bypass surgery, a blood vessel from the patient (e.g., a large subcutaneous vein from the leg or an internal mammary artery) is grafted into the heart artery, bypassing the narrowed or blocked area.
Bypass surgery is performed when stenting is not feasible due to technical nuances, patient anatomy, or multiple lesions.
The most suitable method is evaluated collaboratively by a cardiothoracic surgeon and an interventional radiologist.
Coronary artery bypass grafting has been performed for quite some time and is a routine procedure.
Coronary artery bypass grafting is prescribed when it is truly necessary to improve a person's quality of life, allowing them to walk, move, and work without pain or angina, reducing their nitroglycerin consumption, and extending their lifespan.
At the same time, it's important to understand that all surgeries carry some risks and potential complications, although the risks here are minimal.

2. «Can a large incision in the sternum be avoided during heart bypass surgery?»
— It is possible, but more often coronary artery bypass grafting is performed through the standard approach - through the midline of the sternum.
In some cases, it is possible to perform the operation through a limited access approach - through an intercostal space.
Pros:
- The scar will be smaller;
- There will be no disruption of the integrity of the sternum or chest frame;
- The postoperative period is shorter, as there is no need to wait for bone tissue to heal.
However, minimally invasive surgery carries greater risks, so patients are carefully selected for operations through small incisions.
Requirements:
- Good coronary arteries, sufficiently large in diameter;
- Low risk of life-threatening rhythm disturbances and acute myocardial ischemia during the operation;
- Good anatomical conditions (it is preferable for the patient to have no excess weight);
- Ideally, the absence of diabetes with distal vascular involvement.
Minimally invasive procedures are performed in a very limited field of view. If the surgeon believes that in your case it is better to perform the operation through the standard approach, it is likely that they are guided by the belief that it will be more reliable, safer, and more prognostically effective.
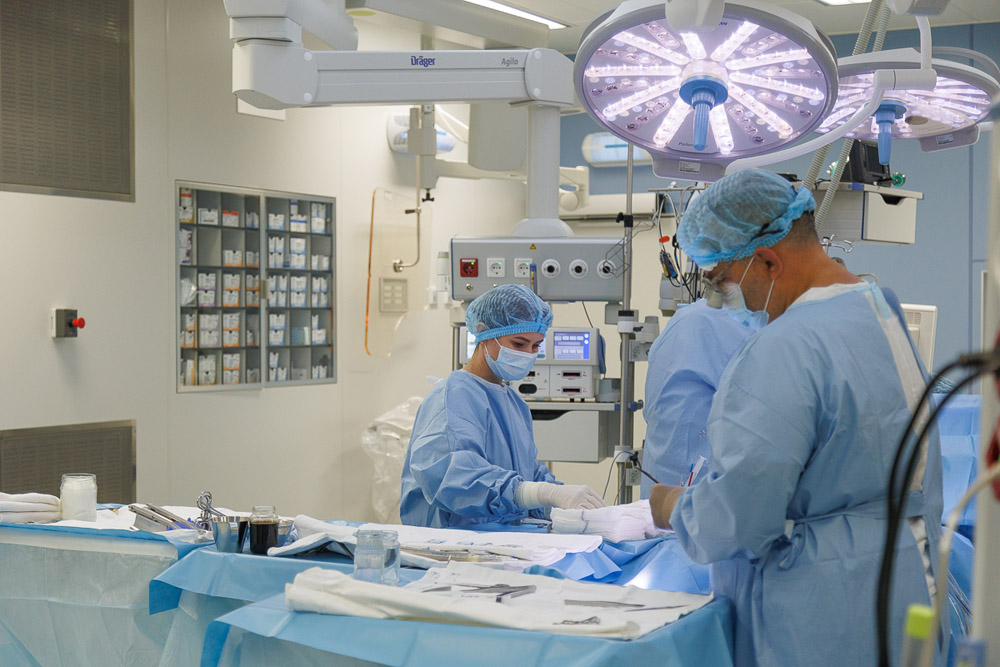
In addition, in most cases, only one artery can be operated on through small accesses. If assistance with multiple vessels is required, an open surgery is typically performed.
It is also worth noting that often the pain syndrome in lateral thoracotomy (limited access) is not less, and sometimes even greater, than with the standard approach. This is because the intercostal spaces may be painful as they are stretched during the operation.
Some surgeons and clinics claim that there is a higher risk of infectious complications with sternotomy (surgery involving the splitting of the sternum) compared to minimally invasive approaches. In reality, in modern operating rooms equipped with all elements for bacterial protection, the risk of infectious complications is minimal.

3. «I want to know how much time it really takes to recover after coronary bypass surgery and return to normal life»
— With standard access, full recovery typically takes 3–6 months. With a lateral thoracotomy approach, it may be shorter.
Rehabilitation can be divided into three stages.
1. When the patient wakes up after the surgery, they should start moving gradually in bed, with rehabilitation specialists assisting them.
From the second day, when the drainage tubes are removed, the patient begins to walk independently and undergoes early rehabilitation, including physical therapy with an instructor.
2. After coronary bypass surgery, a patient can be discharged as early as the 7th day if everything is in order.
After discharge from the cardiothoracic department, the patient is transferred to a rehabilitation unit. Typically, they stay there for 2 weeks, during which their physical activity continues to expand.
3. The third stage is the outpatient phase, lasting up to 2–3 months, until the patient returns to work.
A person can fully return to an active life no earlier than 3 months. This does not mean that they cannot move or walk before that. Walking is encouraged. However, all restrictions are typically lifted after 3–6 months.

4. «What limitations and consequences should one be prepared for?»
- Since a large subcutaneous vein from the leg is often used as a graft, it will be necessary to wrap the legs with elastic bandages or compression stockings for two months to prevent swelling and venous insufficiency after the surgery.
- After the operation, there will be a limitation on shoulder activity for 3-6 months (with standard access) as it takes time for the sternum to heal.
- Discomfort in the area of the surgical incision may be experienced. Often, numbness is felt by patients after taking the internal thoracic artery for grafting. Typically, this numbness diminishes over time.
- Numbness in the area of the inner ankle may also occur after taking the vein, as there is a sensitive nerve nearby. However, this is usually temporary.
- Occasionally, lymphorrhea (lymphocele) may develop, where lymph fluid is discharged from the surgical wound for some time.
It's important to understand that these are not complications but rather features of the postoperative course, meaning they are not dangerous and often resolve quickly.
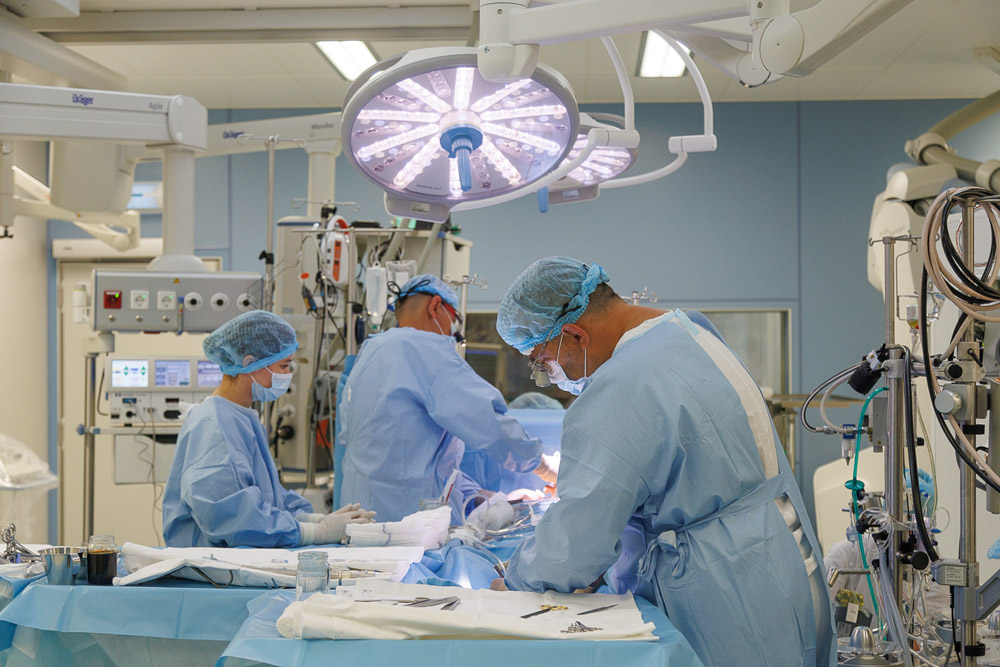
— After coronary artery bypass surgery, your well-being significantly improves, especially if you experienced severe angina, where even simple walking would cause chest pain and breathlessness.
If, prior to the operation, you couldn't walk 200 meters during a 6-minute test, after the surgery, you will find this test much easier to complete. You will immediately notice an expansion in your physical capabilities.

6. «In some clinics, coronary bypass surgery is performed on a beating heart, while in others, it is done on a stopped heart. Which approach is better?»
— It cannot be said that one method is better and another is worse. Simply put, for specific reasons, one clinic's optimal approach is surgery on a beating heart, while for another, it's surgery with the use of artificial circulation. The outcomes are roughly the same.
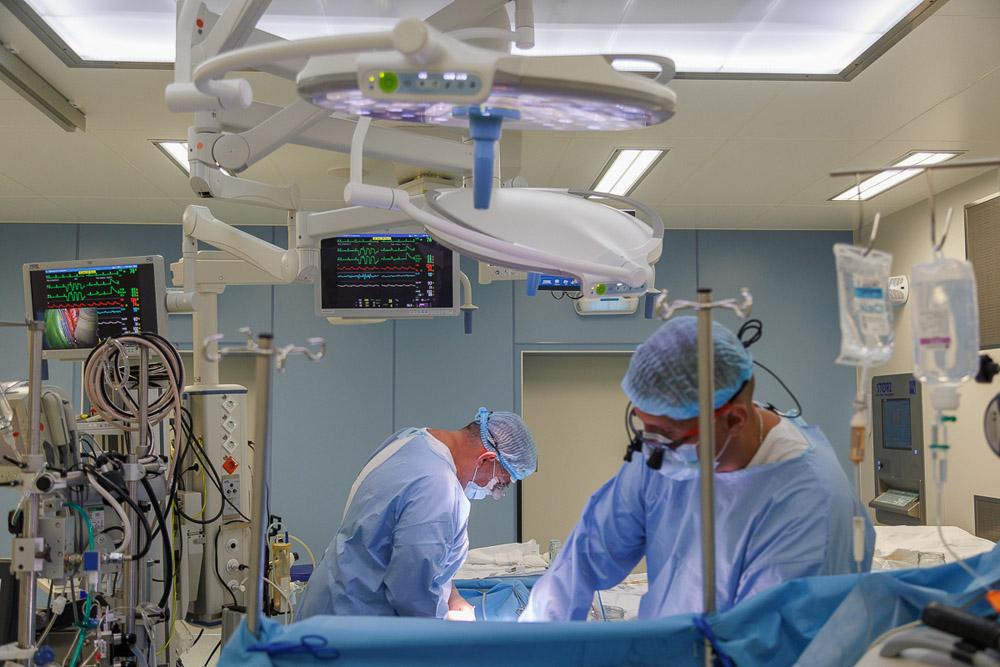
7. «Will a repeat operation be required 10 years after bypass surgery?»
— Not necessarily.
Bypass grafts do indeed wear out over the years. Venous grafts usually have a shorter lifespan compared to arterial ones (the internal mammary artery is considered an ideal choice for grafting).
The average lifespan of venous grafts is approximately 10 years. However, often during examinations, it is discovered that venous grafts continue to function for more than 15 years, while arterial ones can last even longer, beyond 20 years.
Much depends on the condition of the patient's own artery into which the graft is attached. If there is a place for blood to flow, the graft will continue to function for a long time. The progression of atherosclerosis depends on the individual's lifestyle.
It is important to understand that the surgery does not cure the disease itself. It improves blood supply to the heart by creating an additional bypass route around blockages or narrowings. The underlying disease, atherosclerosis, remains.Treating atherosclerosis directly primarily involves lifestyle changes:
- Quitting smoking;
- Following a specific diet;
- Taking medications to thin the blood and reduce cholesterol levels. It's essential not just to take medications but to work with a cardiologist to achieve target cholesterol levels.
If a patient continues to eat indiscriminately, smokes, and does not take medications after the operation, atherosclerosis will progress. Cholesterol plaques will form in other blood vessels, and the lifespan of the established grafts will sharply decrease, as will the patient's life expectancy...
Additionally, other comorbidities like diabetes can contribute to the progression of atherosclerosis.

8. «How long do people live after heart vessel bypass surgery?»
— It's a complex question because it varies greatly on an individual basis. However, research indicates that this operation unquestionably reduces the risk of adverse outcomes from cardiovascular pathology if the patient has involvement of the main artery, stenosis of the left coronary artery stem, or an equivalent condition where all major arteries in the proximal (initial) segments are affected.
Additionally, studies suggest that coronary bypass surgery extends the lifespan of patients with ischemic heart disease and reduced ejection fraction.
But it's impossible to predict how long a specific individual will live after the surgery. I'll emphasize that the operation improves the quality of life, enhances physical activity, and prolongs life, provided that the patient also adheres to the correct medication therapy.

9. «Will I need frequent check-ups after the surgery?»
— Not at all. If there were no complications, it is recommended to visit a cardiologist once a year and undergo routine examinations:
- Echocardiography (heart ultrasound);
- Electrocardiogram (ECG;
- Holter monitoring;
- Stress tests;
- Comprehensive blood tests, including biochemical and lipid profiles.

10. «What happens if coronary artery bypass grafting is not performed?»
— In cases, as described above (stenosis of the initial segments of major coronary arteries), there is a risk of sudden coronary death. We emphasize that the surgery is necessary for life-saving reasons.
If a patient still refuses for some reason, the only option left is to refer them to a cardiologist for the prescription of optimal medical therapy, which includes the use of blood-thinning medications (possibly a three-component regimen), medications that lower cholesterol levels, and medications that regulate blood pressure.
Interviewed by: Kristina Holovyichuk
Photo: Elena Gordeychik, Alexander Zadorin
103.by



