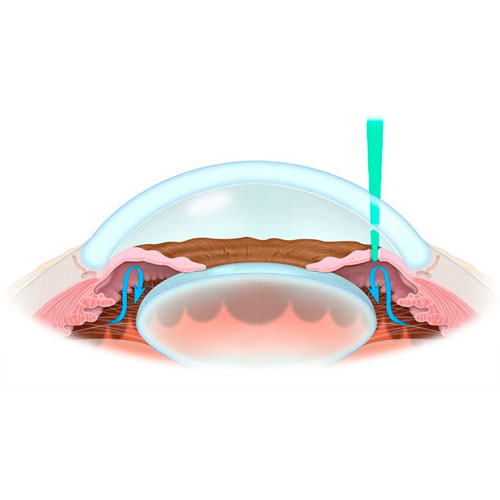
Symptoms of glaucoma were described as far back as in year 400 BCE by Hippocrates. Active study of the disease started during the late 19th century, however, even now ophthalmologists continue the search for its exact cause.
The term “glaucoma” includes a broad group of eye disorders that have different clinical courses; the most evident of them all, however, is elevated intraocular pressure. If not treated properly, glaucoma may result in complete loss of eyesight.
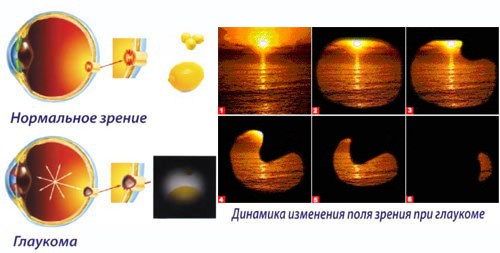
According to data gathered by WHO, approximately 13.5% of all the blind persons lost their eyesight because of glaucoma. Gradually and irretrievably, the patient loses eyesight, with peripheral vision being the first. Regular comprehensive examinations performed by an ophthalmology specialist help to identify the disorder, determine proper treatment and control its effectiveness.
Types of glaucoma
In terms of eye fluid efflux, the following types are distinguished: closed-angle glaucoma, open-angle glaucoma and mixed glaucoma.
Depending on the cause and time of glaucoma development, it may be classified as:
- primary; and
- secondary.
Besides the above, there also are:
- congenital glaucoma; and
- juvenile glaucoma.
Open-angle glaucoma develops discreetly, and accounts for 90% of all the identified cases. This type of glaucoma is characterized by that the access to the drainage system is unobstructed, but the function of the eye fluid efflux system is impaired which results in a gradual increase of intraocular pressure, sometimes over the course of several years. As the result, the patient may loose eyesight imperceptibly.
Closed-angle glaucoma is noted for its aggressive development which is noticed by the patient. Access to drainage channels is interrupted and intraocular pressure increases rapidly causing acute pain in the eyes and headaches, as well as reddening of eyes and sharp decline of visual acuity.
Congenital glaucoma is a pathology related to abnormal development of the eyeball. This disorder is revealed during the first several days or month after birth.
Symptoms of glaucoma
Increased intraocular pressure may be evidenced by acute painful sensations in the eyes, halos around light sources, feeling of heaviness, and cloudy vision. Eyesight is impaired, especially in the twilight. Gradual tunneling of vision, down to a small spot, is noticed; an edema of cornea and reddening of the anterior chamber of the eye may develop. The pupil dilates and does not react to light.
In most cases, however, the patient does not even suspect they have glaucoma. In fact, not every physician is able to identify a developing glaucoma, even with the use of the most advanced equipment.
Causes of occurrence and development
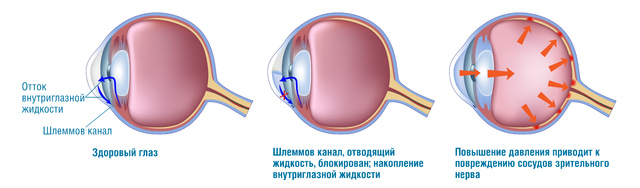
Our eyes maintain ocular pressure though proper and precise distribution of fluids. When the supply and efflux balance is upset, pressure starts to rise within the eye and all structures of the eye are excessively stressed. This is followed by obstruction of blood circulation and neuron death; no signal passes to the brain and the person loses eyesight.
Modern medical science identifies three risk groups:
- Senior persons. The majority of established cases fall upon the advanced age group (60 and older).
- Racial specifics. Prevalence and severity of the disorder in representatives of the Caucasian race is noticeably lower than in the Negroid race.
- Retina disorders. Physicians frequently associate development of glaucoma with retina disorders.
- Myopia (shortsightedness). Persons affected by myopia often have an elevated opthalmotonous pressure. This tends to damage the structure of the eyeball and provoke the increase of intraocular pressure.
- Hereditary particularities. Direct relatives fall into the risk group. The exact relationship and the inheritance scheme have not been revealed. To confirm hereditary transmission, the patient needs to be observed over a period of several years. According to the latest data, the probability of development of glaucoma in a patient's children is 4%, and in brothers and sisters -- 10%.
Most frequently, the disease is manifested in persons over 65 year of age. At ages of 40 to 55 years, glaucoma is revealed in approximately 0.1% of the planet’s population. Among infants, one case of congenital disease occurrence is noted in 10 thousand children.
To prevent the development of the disease, medical specialists recommend:
- Visit an ophthalmologist for a study of eye structures.
- Regularly measure intraocular pressure and have your vision field checked.
- Control your visual acuity independently.
STAGES OF GLAUCOMA THERAPY
The initial stage of glaucoma therapy after it was diagnosed is pharmaceutical therapy of the patient, that is, instillation of eye drops to reduce intraocular pressure.
If the therapy does not produce the required result, laser or surgical intervention is required.
Unlike eye drops that serve to maintain fluid balance within the eyeball, a surgical procedure enables full recovery of this balance. This is a radical but effective and resultative procedure.
Remember! By postponing a visit to an ophthalmologist you risk the health of your eyes.
INDICATIONS FOR SURGICAL TREATMENT OF GLAUCOMA
- Elevated intraocular pressure which cannot be treated medicinally, and associated progressive deterioration of visual functions condition (alteration of filed of view, impairment of the optic nerve disk and progressive deterioration of visual acuity).
- Acute exacerbation of glaucoma.
SURGICAL TREATMENT OF GLAUCOMA AT THE RCMC
Sinus trabeculectomy in cases of open-angle glaucoma
Surgical treatment involves formation of an additional ocular fluid efflux passage. This is done by excising a small piece of the sinus drainage system and the trabecula. This procedure is the international golden standard in glaucoma therapy.
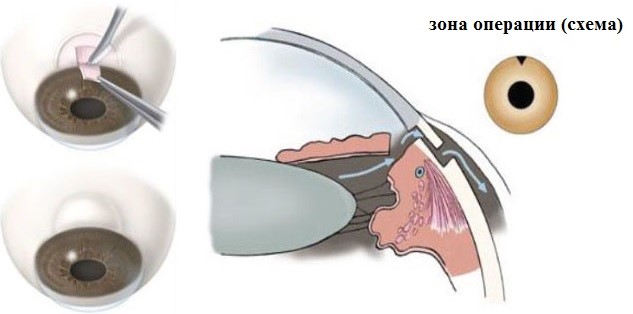
Iridocycloretraction in cases of closed-angle glaucoma
Iris which prevents the efflux of fluid from the ocular anterior chamber, is restored at its original position, and is fastened there.
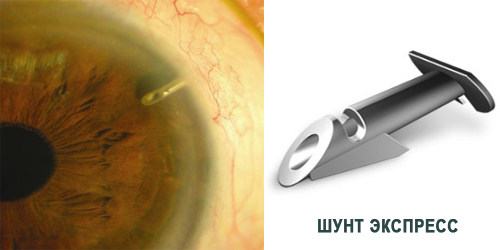
Drainage device (Ex-Press shunt by Alcon and Ahmed valve) implantation operations
At out Center we also perform additional glaucoma therapy procedures (implantation of drainage and valve devices) at a high professional level.

CONTRAINDICATIONS
- certain concomitant eye disorders;
- decompensated systemic diseases;
- cases when the risk of visual acuity impairment exceeds potential benefits.
HOW TO GET SURGICAL TREATMENT OF GLAUCOMA AT THE RCMC
- Call the Contact Center to make an appointment with an ophthalmologist
- Conclude a contract for the provision of paid services at the registry.
- Pay the invoice at the cash desk of the RCMC or via ЕРИП (SSIS: Single Settlement and Information Space)
- Come to the consultation on time.